Calderdale Birth Centre

How to find us: Facing the main entrance at Calderdale Royal Hospital, take the outside path towards the right of the entrance which leads directly to the Birth Centre entrance
Opening Hours: 24 hours a day 7 days a week
Phone: 01422 224417
Visiting Times:https://www.cht.nhs.uk/patients-visitors/visiting-times-from-march-2020/


Our Birth Centres are small and friendly offering a comfortable environment for birth. They are staffed by experienced midwives and maternity support workers who are skilled in facilitating natural birth. We provide one to one care for women and their partners, supporting active birth, water birth and hypnobirthing techniques.
Research suggests that having your baby in a Birth Centre can increase the chances of achieving a normal birth and reduce the risks of intervention, such as, assisted birth, episiotomy, need for medicinal pain relief and caesarean section (Birthplace study, 2011). Women who have their babies at a birth centre are more likely to birth in water and report higher levels of birth satisfaction.
Calderdale Birth Centre is an ‘alongside’ unit which means there are obstetric services within the same building. Should you need input from the Obstetric team during your labour or birth you would be transferred to labour ward on the second floor of the hospital which would take around 5 minutes.
To care for you safely the birth centre is only suitable for ‘low risk’ pregnancies including:
- Up to fifth pregnancy
- Uncomplicated previous births
- Spontaneous labour at 37 – 42 weeks
- Singleton pregnancy
- Uncomplicated pregnancy
- BMI 18 – 35 (first baby)
- BMI 18 – 39.9 (if previous uncomplicated birth)
- Will not require an epidural (transfer to Labour Ward if needed)
To facilitate natural birth we encourage use of active birth equipment and techniques such as upright positions and mobilisation. To make you comfortable we use massage, heat packs, waterbirth and lots of support. If needed, we can offer Entonox (gas & air), Pethidine or Meptid when you are in established labour.
When to attend:
If you are planning to birth on Calderdale Birth Centre, please always phone before arrival so that we can have your room and midwife ready to welcome you.
If you are 37 weeks pregnant or more and think your waters have broken or labour has started, you can phone us 24 hours a day for advice and support. You can discuss what is happening with a midwife and agree when would be the best time to come to the birth centre.
If you are under 37 weeks please phone Maternity Assessment Centre directly.
What to expect:
Please bring your maternity notes and your bags packed for labour and for baby. A Midwife or Maternity Support Worker will show you to your room and help you settle in. You will have your own room with en-suite bathroom facilities and you are welcome to bring in your own music and items that will help you to feel comfortable. Your Midwife will perform a full assessment with your consent which will include a review of your medical history and pregnancy, your blood pressure, urinalysis, palpation, and vaginal examination if necessary.
You will be provided with one to one care when you are in labour and we encourage you to bring the birth supporter of your choice.
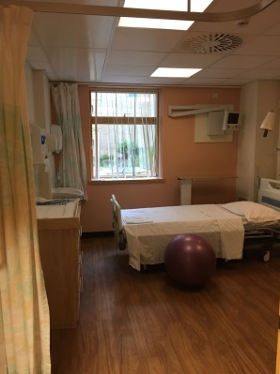
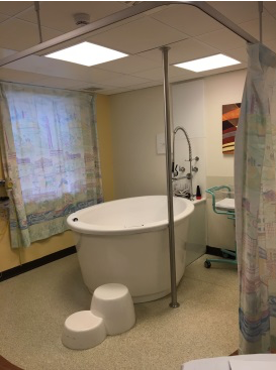
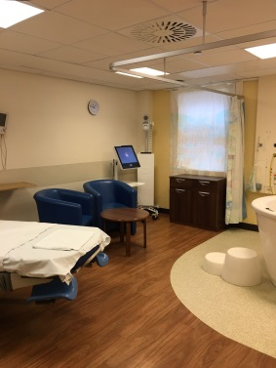
Guest facilities:
- Kitchen with kettle & microwave
- Fruit juice, tea & coffee, biscuits, toast.
- Active birth equipment
- Birthing pools
- Garden space for early labour
- Contemplation and prayer room on site
Meals
Whilst you are staying with us your meals will be provided. Please let us know of any dietary requirements on admission. We have facilities for birth partners to make hot drinks & snacks and there is a café and a restaurant in the hospital Monday to Friday.
After the birth of your baby
If you have birthed in one of our pool rooms we will move you into a different en-suite room for the remainder of your stay.
If this is your first baby it is usual to stay with us for at least one night so that we can support you with feeding however, if you wish to leave earlier, this can be facilitated. Whilst you stay with us you can expect:
- Care from a named midwife
- Daily checks of mother and baby
- Baby to have a newborn hearing screen
- Baby to have a full newborn examination after they are 6 hours of age
- Baby to have BCG vaccine if indicated
- A Bounty welcome pack (please note this is optional, let ward staff know if you do not wish this service)
- To be consulted about your discharge arrangements/follow up
Feeding your baby
We offer round the clock feeding support specific to you and your baby’s needs.
Breastfeeding – All our staff are trained to support breastfeeding. Please call for assistance and support as you need it, day and night.
Bottle Feeding – If you have chosen to bottle feed, please bring in two bottles and your powdered milk. We will support you with feeding and show you how to sterilise and make up a feed. We provide a cold water sterilising unit for your exclusive use.
Going Homeand ‘6 hour discharge’
We aim to get you home as soon as possible but only when it is safe and appropriate to do so, depending on the needs of you and your baby. Although we plan your discharge in advance, your discharge home is reliant on a number of processes which can take some time to complete once the decision is made.
Some mothers wish to go home as soon as possible and if all is well you may be supported to have a discharge to home from hospital from around 6 hours following the birth of your baby. If this is the case the full neonatal examination cannot be carried out before the baby is 6 hour old, so discharge will actually take place more than 6 hours from the time of birth.
Follow Up
Your community midwife, GP and health visitor will be notified of your discharge home with baby and you can expect to hear from a community midwife the following day. Please ensure we have the correct discharge address and contact phone number so the community midwife can contact you. If you have any problems once home you can still contact the ward for advice until your midwife has discharged you from our care.

















